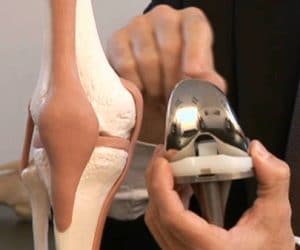
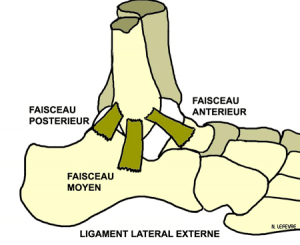
Lesion of the anterior cruciate ligament in children.
The pure ligamentous injuries of the child are certainly underestimated, with the commonly accepted concept of more fragile bones and ligaments of the concept lesions preferentially affecting domestic growth plate in epiphyseal and metaphyseal rather than ligaments.
Yet before a LCAE lesion in children, unless you have a child captivated by video games, most of these children practice sports daily basis pivot physical activities, see pin contact, hardly observing soon as the acute episode happened precautionary instructions that may be required to do.
Anatomic laxity are often important even less well tolerated functionally they can occur on land of physiological general joint hypermobility.
EPIDEMIOLOGY
Epidemiologically, LCAE lesions are rare.
A company epidemiological survey for the symposium of the French Society of Orthopedic Surgery and Traumatology ( “SOFCOT” November 2006) on two pediatric hospitals (Lyon and Tours) out of 2005 found only 3% of knee injuries (single wound fractures contusion or 716 knee injuries on 24855 pediatric emergencies.
Of these 716 injuries of the knee, 115 correspond to pure ligament injuries (3%) mainly affects mostly internal peripheral ligaments, with not 421 distribution, but 721 (7M, 2L, 1 LCAE) or 12 cases of lesions the LCAE diagnosed.
They are rare before 9 years, 7 years before exceptional rather affect girls before age 12 and occur mainly with the waning of sports injuries.
US studies (BRADLEY 1980 Mc Caroll 1988) found a frequency of 1.5 to 4% LCAE of injury occurring before the age of 15 years with respect to all diagnosed LCAE lesions.
Done newer, pure LCAE injuries are also common if not more than traditional bone lesions of the tibial spines in children as reported BRACQ in 1996 (survey of the Western Orthopaedic Society in 1996).
In Scandinavian countries it is estimated the incidence of this lesion 1/100 000 children per year.
The practice survey conducted in France in 2005 for the November 2006 symposium suggests the occurrence of 350 to 400 cases per year of which 150 operated about a year.
We can estimate that in our practice we can be confronted with this problem once or twice a year.
EVOLUTION OF NATURAL DAMAGE IN CHILDREN LCAE
Most of the time, the natural reflex pediatricians, sports doctors and orthopedic consultation is to opt for a temporary solution to consider radical treatment in growing finished, because everyone is well aware of the potential vis-à-vis risk growth techniques we use common ways of adults.
The frequency of meniscal lesions during the initial accident led some and may even lead to irreparable, namely meniscectomy on unstable knee.
Yet the poor prognosis of the natural evolution of a LCAE lesion in children is now well established.
Regarding the functional instability secondary to LCAE lesion in children, Romain CIL, through a meta analysis of the literature in 2000 found 92% of secondary instability if conservative treatment against just 10% of secondary instability in case of intra-articular reconstruction of LCAE.
Despite the legendary healing power of children, simple sutures torn LCAE lead in most cases to failures, the role of extra-articular plasty waiting like Lemaire is entirely random.
The same findings were found as part of conservative treatment awaiting the end of growth, by (?):
- GRAF (Arthroscopy – 1992) about 12 cases with a mean of 2 years include 100% of secondary instability.
- Mizuta (JBJS – 1995), about 18 cases with a mean score of 89% secondary instability.
Alongside this secondary instability, we must emphasize the frequency quite unusual meniscal lesions they are primitive (mainly affecting the lateral meniscus) or secondary:
- GRAF (Arthroscopy – 1992): 75% of initial meniscal lesions
- Mizuta (JBJS -1995): 78% of initial meniscal lesions
- Chotel – BELLIER: 50% of initial meniscal lesions
- WOODS: 46% of secondary meniscal tears
- ARONOWITZ: 68% of secondary meniscal tears
- The secondary meniscal lesions occur in 75% of cases in the year following the injury LCAE.
Even more serious is the presence of genuine signs of osteoarthritis worsen steadily over the years of decline (3 years, 6 years, 8 years) while it is still only a teenager:
- Mizuta (JBJS – 1995) note 3 years follow in middle-age teenager 16 years 61% of radiographic abnormalities including 18% joint space including internal femoral tibial
- AICHROTH (JBJS – 2002) note 6yrs decline in middle-age teenagers aged 18 ½ to 43% with radiographic abnormalities in 33% of cases of joint space narrowing
- Kannus (JBJS – 1988) had already noted these radiographic abnormalities to 8 years of decline in 57% of cases.
KNEE LCAE GROWING
EXPERIMENTAL DATA
Yt why so many still reluctant to offer surgery before this admittedly rare lesion, but if the pejorative potential.
Because it occurs in a growing knee.
A number of experimental studies have revealed major concepts essential to know qi is being proposed ligamentoplasty LCAE in children.
The work at the Rabbit Guzzanti in 1994, confirmed by Jannarv in 1998 showed that achieving tunnel through domestic plate does not cause secondary growth disturbance provided that small (less than 12% diameter of the tibial physis to the level less than 11% of the diameter of the femoral physis level) in the center position
Stadelmaier (1995) in dogs, and Seil (2001/2006) in sheep have shown that filling a tunnel trans physeal by a tendon graft protected the risk of secondary epiphysiodesis, Seil also emphasizing the harmful role of systems trans physaires fixing (screw absorbable interference particular).
Given perhaps less known, too much tension for attaching a tendon graft through the snails can lead to slower growth (tenodesis effect grafts) experimentally proved by ONO in sheep (1998) and Edwards in dogs ( 2001) confirmed by KOCHER in 2002 (retrospective clinical study) with the appearance of genu valgus secondary in case of extra articular plasty kind Lemaire (even without lesion perichondrial ring).
The construction of a tunnel in trans physeal tibial anatomic position in the child, without risking cause side growth disorders, is possible provided that certain rules are more vertical than in adults, remote domestic plate and the area of ??the TTA, the diameter must not exceed 10% of the diameter of the tibial plate married.
Femoral level, in the same way, achieving a size physeal trans tunnel adapted to the size of the femur is still possible (anatomical location), but care must be taken not to damage the perichondrial ring source of secondary axial deviation: it is necessary to keep a safety distance of 2 mm from the posterior cortex (for example, a tunnel of diameter 6 mm, the femoral viewfinder must have an “offset” of 5 mm)
This risk increased in femoral encourages some to favor a pass over the top but at this time there and not isometric also not without risk to perichondrial ring but also the possibility of secondary verticalization line Blumensath (s roof notch) as found Bonnard supporter of the technique of soft baguette in children.
It is therefore fundamental that the surgeon have to support a LCAE lesion in children know the rules of pediatric orthopedic surgery before offering anything as treatment and avoid these side coarse errors sterilization of the TTA, deviation secondary or even axial length inequality end of growth as members sometimes reported.
This includes avoiding all means of fixing grafts in reintegration through tunnels domestic plate (interference screw whether metal or bioresorbable) and cortical fixation focus away from growth plates.
CLINICAL
1) CLINICAL DIAGNOSTICS
The clinical picture of a lesion of the child’s LCAE is hardly different from that of adults.
The injury LCAE occurs in most cases after a sports accident (training, competition or leisure) and given the level of practice of sports in France occurs most often during football practice or winter skiing.
notable difference, however, data interrogation, especially concerning the traumatic mechanism, are more difficult to say that the child is young; Sometimes we find a notion of cracking and swelling with secondary functional impotence, but this is not very characteristic and most of the time, it is the diagnosis of post-traumatic hemarthrosis occurring in a child more or less young.
Outside the epiphyseal fractures, be aware that major causes of post-traumatic hemarthrosis of the child are patella luxation (usually on locoregional dysplasia), the osteochondral lesions or avulsions and chondral lesion LCAE (in 25-40% of cases according to published series Kellemberg 1990 / Chotel 2004).
First of all, before the clinical picture of posttraumatic hemarthrosis should be carried out a comparative radiological assessment of the 2 lap (at least 4 basic shots: front, side, and intercondylar indentation patellofemoral parade at 30 ° always feasible even in the context of the emergency) before further clinical examination.
The radiological assessment makes it possible to eliminate fractures (including fractures of the tibial spines) cut away bone (medial border of the patella through dislocation, bone and ligament tear), the osteochondral fractures condylar etc … ).
Then, the recovery of the clinical examination allows a more or less easy to suggest the diagnosis of ligament injury pure LCAE, possibly after puncture-evacuation of hemarthrosis in conditions of strict aseptic technique.
This diagnosis is based, as part of the emergency, the finding of a sign Lachman more or less easy to interpret, especially as the child has a ligamentous laxity character.
2) IDENTIFY THE KNEE IN RELATION TO ITS GROWTH REMAINING
The first thought that must have when a suspected injury to a child LCAE posttraumatic hemarthrosis is to situate this knee over its remaining growth
2/3 of the growth at the lower member is from the knee, and it must disassociate growth remaining at the knee and growth remaining at the level of the whole body
Conventionally known knee growth areas: marital plates femoral and tibial level and area of ??the tibial tuberosity (including sterilization secondarily causes a knee-recurvatum with modified tibial slope particularly important that sterilization occurs earlier).
Over 2/3 of growth in lower limb length returning to conjugal plates knee, 60% come from the femoral plate domestic and 40% of the domestic tibial plate.
This growth is not only in length but also in thickness with the very special role of perichondrial ring true stabilizer epiphyseal metaphyseal whose peripheral damage will result in axial deviation (1 mm = 1) varus or valgus depending on which side of the reached.
.
Among the clinical and para-clinical evidence to place the knee in its residual growth, chronological age is certainly not a factor to be taken into account, individual variations in growth based on chronological age being far too important before 16/18 years to reflect this.
Analysis of secondary characters pubertal (Tanner classification) is definitely an extra quite interesting; examine the axillary and pubic hair is part of the clinical examination of a child with an injury LCAE (without however shocking it may seem).
The menarche in girls is an interesting landmark but be wary especially for the sporty girl high level (onset delayed period, offset growth in time).
In fact, the best criteria of residual bone growth is bone age, analyzed on the radio of the elbow and / or wrist and hand. Its difficult interpretation requires the intervention of the radiologist.
But there is a major difference in the residual bone growth, bone age equal between the girl and the boy; and at 13 years of bone age, residual growth in the knee is less than 1.5 cm (almost finished) with the daughter as she left May-June cms in boys.
In practice, because of easy interpétation used systematically in the monitoring of scoliosis in children, the test RISSER, analyzed on an AP view centered on the iliac crest (analysis of secondary ossification of iliac crest) may be applied at the knee to determine the potential residual growth of the knee in children.
The ossification of the iliac crest starts with the appearance of the anterior ossification core at the anterior superior iliac spine (Risser 1) and then continues with a calcic edging end pointing toward the posterior superior spine ilique (Risser 2). When calcium rim reached the iliac posterior superior spine of the test Risser is 3, then the melting of the calcium border with the rest of the iliac crest is back to front (Risser 4). When the merger is complete bone leading to the anterior superior iliac spine (Risser 5) the aggregate of the individual bone growth is complete.
At the knee, whether at the girl or boy, a test RISSER 3 corresponds to a bone growth knee almost complete, residual growth being less than 15 mm (this test Risser 3 appears at the girl a bone age of 13 years 6 months and in boys for a bone age of 15 years 3 months).
TO BEHAVE
What then is the best therapeutic management today before a post traumatic hemarthrosis of a young child /- where is suspected lesion LCAE which was located potential residual growth at the knee.
Certainly today, and certainly even more in the future, the realization of emergency MRI to confirm the diagnosis of ligament injury in children LCAE and specify any particular meniscal lesions.
Without this emergency MRI, at the symposium of the SOFCOT 2006 were a pragmatic attitude of prudence dramatization: landfill (splint, rods) and reconsideration 15/20 days
Yet a number of arguments can justify, particularly in young high-level athletic child a more aggressive stance, conducting arthroscopic certainly all the more difficult as the child is young, but will allow a more accurate lesion diagnosis possible and appropriate treatment for injuries encountered.
Gaulrapp (2006) over a period of 10 years (1982: 1992) 457 performs arthroscopy in children between 3 and 16; it found 20% of injury LCAE similar percentage already held by Kellenberg (1990).
Stanitski (1994) and more recently Chotel in France in 2003 found a LCAE lesion frequency of 45%
For our part, given the impossibility of using MRI in emergency in 4/5 days, arthroscopy appears quite justified.
It allows the assessment of the lesions intra exact knee joint, treat the associated meniscal lesions found in 50% of cases, treatment dominated by conservation meniscal capital (suture, ie let up stable meniscal tears)
Exceptionally it will allow the diagnosis and treatment of avulsions LCAE floor or ceiling with suturing techniques such Marschall with known good results can be also enhanced on a national law guardian (technique used in the CHO adult in the 80s, adapted to the rules of pediatric surgery).
The decision of such an attitude requires a course in as rigorous and honest information as possible actions that can be taken to achieve in this vis-à-vis gesture of the child and its parents.
In some cases it may even be necessary to perform a ligament.
Ligamentoplasty THE TECHNIQUES USED IN CHILDREN LCAE
In terms of ligamentoplasty LCAE in children, there are several possible techniques, the best is certainly the one that has the best command.
We can distinguish them based on compliance or non-marital plates during their realization
DIFFERENT TECHNIQUES
THE PROPER TECHNIQUES DOMESTIC PLATES
This is the most ancient techniques they use:
- Hamstrings (LISCOMBS / 1986 BRIEF / 1991)
- The technical patellar tendon so-called soft baguette mainly used in France described by the team Clocheville in Tours (BONNARD)
- The fascia lata (described by Kocher in 1980) reported by Jaeger in France (2001)
These techniques have the prerogative of anticipation, follow the growth plates but not as part of a reconstruction LCAE perfectly congruent.
TIBIAL transphyseal TECHNICAL ONLY
Depending on the used graft, it is isometric LCAE reconstructive procedures through the conjugal tibial plate so as to have an anatomical tibial anchoring, but respecting the femoral conjugal plate while being anatomical femoral level (the femoral tunnel epiphyseal seat below the growth plate, they are more difficult to realize that the child is young).
They use either hamstrings hamstrings (ANDERSON / 1995) the quadriceps tendon (Chotel / 2003 / Lyon Technique) or even grafts banks (ANDREWS / 2001)
TECHNIQUES THROUGH PLATES AND femoral TIBIAL GROWTH
They have grown because of the ease of use of hamstring hamstrings (hamstring) and were reported by SIMONIAN (1999) and AICROTH (2002)
They are perfectly congruent, but should avoid irritating the perichondrial ring at the posterior superior edge of the notch.
MAJOR TECHNICAL DIFFERENT THESE PRINCIPLES
Whatever the technique used, it must obey the principles of pediatric orthopedics:
- Know where marital plates and achieve the passage of ligamentoplasties without exposing these growth plates located.
- Do not use with inert fixing transphysaires ligamentoplasties passing through the growth plates (no interference screws)
- Fixing of transplants in cortical or cancellous status remotely growth plates
Regarding the postoperative, certainly according to the technique, be aware that postoperative stiffness “does not exist” in children and that we should not hesitate to use postoperative assets non-removable articulated or not, keep 6-8 weeks (see 3 to 4 months in hypermobile children keeping a safety flexion).
The accelerated rehabilitation protocols are not appropriate for children and you have to wait for the maturation of the graft before allowing the resumption of sports.
PERSONAL SERIES
From 1989 to 2005, we faced 48 LCAE injuries in children aged 7-15 years:
- One aged months to 11 years (bucket handle the associated dislocated medial meniscus was sutured without specific gesture on LCAE immobilized by resin for six weeks, followed for 2 years, no functional complaint despite persistent anterior laxity then lost sight).
- 7 children ages 11 to 13 years
- 40 children aged 14 to 15 years)
7 children have been followed over six months (lost to follow).
36 children were operated (21 girls and 15 boys) in a variable period of 15 days to 3 years.
The intervention has been performed RISSER 3.
2 children are currently awaiting surgical treatment.
Apart 3 children who underwent arthroscopic semi-emergency, which has achieved sutures kinds Marshall (1 avulsion the femoral, the tibial avulsion 2 level) with a decline of 3 to 7 years with a great result IKDC .
For those who were operated on, it was prescribed orthotics articulated protection (without much hope, because the longer the period of limitation is, the less children wear their brace) and were exempt from any sporting activity involving pivots at knee (again with a more or less respected efficiency because, unless you have children captivated by the game consoles they submit their knee pivot constraints in their simple -Courtyard leisure activity or recreation other).
In terms of surgical technique, considering an intervention to RISSER 3, without potential risk with respect to growth, the technique used was transphyseal femoral and tibial isometric distinguished into two periods according to ligament reconstruction performed arthroscopically:
- Technique using a bone graft bone patellar tendon according to Rosemberg technique (6 children between 1989 and 1994)
- Technique using hamstring (30 children between 1995 and 2005).
All these 36 children were revised growth ended with a decline of 1 to 8 years.
Analysis of primitives associated meniscal lesions found during the initial arthroscopy or MRI assessment performed in emergency (48 cases):
- Absence of meniscal lesions in 24 cases or 50% of cases
- Meniscus lesions considered steady (less than 15 mm in length) and left in place: 10 cases
- Partial meniscectomy in 8: 6 concern the lateral meniscus (unstable lesions oblique back of the slot of the popliteal) 2 concern the medial meniscus.
- Meniscal sutures in 6 cases, 3 in the medial meniscus, 3 at the lateral meniscus.
Analysis of meniscal tears “secondary” at the time of reconstruction gesture LCAE (36 cases with a mean period of 18 months from the initial accident):
- Absence of lesions in 13 cases (66% of secondary lesions)
- Meniscal sutures in 18 cases (13 on the medial meniscus, 5 on the lateral meniscus) with 4 cases of meniscal suture failure in two postoperative years
- Partial meniscectomy in 5 cases (3 lateral, medial 2) including 2 primary meniscal suture failures made during the contemporary arthroscopy of the lesion.
Analysis of secondary stability (IKDC score) (36 cases with a decline of 1 to 8 years):
- For recurrent anterior laxity in 2 cases (biological failure of graft integration occurring on hypermobile children (physiological recurvatum above 10 ° insuffsamment not constrained in the postoperative period.
- 1 case of traumatic rupture of the transplant true to 5 years follow the waning of a new knee sprain in a young woman practicing handball.
- No failures in the initial short series using the patellar tendon as a graft
- Score IKDC A or B in 81% of cases.
To the extent that all the children were made to RISSER 3, no secondary bone growth disorder was found.
GROWTH DISORDERS SECONDARY TO SURGICAL TECHNIQUES USED IN CHILD
In terms of secondary growth disorders, can now be based on two multicenter studies: the US study of Herodicus group (practical study on 140 surgeons reported by KOCHER 2002) and the French study SOFCOT 2006.
The US study, based on criteria “wide” Growth Disorders analysis (axial deviation of the lower limb above 5 °, length discrepancy in the lower limbs than 15 mm).
It reported 11% of “major” growth disorders without it the reports to a defined technical nor specifies the notion of secondary interventions related growth disorder:
- 11 cases of secondary valgus femoral
- 3 cases of tibia recurvatum by sterilization of TTA
- 1 case of unequal length 30 mm
The French study is based on analysis strict criteria concerning 92 complete files in their analysis (over 139 cases) including the realization of direction finding, strict profile face radios study include the orientation of the line Blumensath to flexion of the femoral epiphysis etc … and more stringent criteria (unequal length greater than 10 mm higher than 5 ° angular disorders …)
It reported 12% of secondary growth disorders (11 cases out of 92), some cases can have several simultaneous growth disorders according to the plane in which the analysis was done (frontal, sagittal, length …)
- 4 cases of femoral valgus including one case that required reoperation
- 4 cases of bending of the femoral epiphysis (Clocheville technique)
- 7 cases of verticalization line Blumensath (Technique Clocheville)
- 5 cases of tibial malalignment: 2 varus and valgus 3
- 2 cases of unequal length greater than 10 mm (including the case of valgus operated femur).
If we must not underestimate it vis-à-vis the growing risk in case of intervention on the LCAE on one knee in growth, they appear both in number and seriousness much less harmful (except exception) that disorders caused by the natural evolution of a LCAE of injury in the non-operated child (over 30% of radiological remodeled arthritic type 8 years of decline)
CONCLUSIONS
The injury LCAE in children is more common than we think.
This raises the lesion diagnosis to post-traumatic hemarthrosis of the knee in children who should be as specific as possible (emergency MRI, failing arthroscopic balance sheet).
Functional treatment is only a temporary solution you need to know when not to extend anterior laxity proved.
Extra-articular plasty Lemaire kind, advocated a time in France, are no longer appropriate.
Surgical indications may be put in the child before the end of growth (before RISSER 3) especially among young people belonging to high-level sports centers or in particularly unruly children safely significant vis-à-vis the residual growth of the knee.
The frequency of initial meniscal lesions and secondary fortiori encourage this attitude “aggressive” This is all that we can expand meniscal preservation indications (sutures or respect of stable lesions).
The specifications do not have this problem after RISSER 3, growth on the knee can be considered complete.
The management of such a problem requires a thorough knowledge of pediatric surgery and arthroscopic technique:
- It is more or less knee small narrow notch
- Must know the location of domestic plates without ever exposing the
- Must perfectly master the repair technique chosen
- The meniscal economic dogma must always be present.
And do not forget to provide all the information beforehand to parents (especially in the case where an arthroscopic assessment is proposed to posttraumatic hemarthrosis and where the repair actions can be “caught” in the moment).
BIBLIOGRAPHY
A comprehensive bibliography will be available on the two articles of references:
Kocher MS, HS SAXON, HOVIS WD, RJ HAWKINS
Managment and complications of anterior cruciate ligament injuries in skelettaly immature patients: survey of the Herodicus Society and the ACL Study Group
J Pediatr Orthop, 2002 Jul-Aug; 22 (4); 452-457
Editor F.BONNARD
Symposium “LCAE in children”
SOFCOT, 82nd Annual Meeting, November 2006
RCO, 2007, Forthcoming
Doctor Nicolas LEFEVRE, Doctor Serge HERMAN, Doctor Yoann BOHU. – 3 janvier 2015.